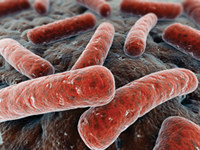
Bacteroides fragilis, a common
boarder in the human gut, may play a role in preventing
colitis |
Rather than being passive guests
in the gut, certain bacteria appear to play a crucial
role in the prevention of diseases such as colitis,
new research in the May 29 issue of Nature suggests.
Scientists hope that this finding will help develop
new approaches to treating inflammatory bowel disease
(IBD).
Zeroing in on the microbe Bacteroides
fragilis, a common boarder in the human gut, the
researchers discovered that this bacterium excretes
a sugar molecule that tampers with the immune system
of its host. When the organism was missing in the gut
microflora of mice bred to develop colitis, the rodents
came down with severe symptoms of the disease. But they
were virtually disease-free when the microbes were present.
"This is the first proof that an
imbalance in normal gut bacteria can cause colitis,"
study author Dr Dennis Kasper, a physician microbiologist
at Harvard Medical School, told NRM. Until now,
researchers had assumed that the microbe in question
did neither harm nor good, but it turns out that B
fragilis is a real team player. The bacterium produces
a sugar molecule, polysaccharide A (PSA), that stimulates
the release of anti-inflammatory cytokines in the host's
bowel. It also suppresses the release of pro-inflammatory
substances in the gut.
MOLECULE
MADNESS
To check whether PSA really was what was protecting
the colitis-prone mice from disease, the researchers
purified the substance and fed it dir-ectly to the animals.
What followed was a bit of a eureka moment. "If you
give them pure PSA, they don't get col-itis," beams
Dr Kasper. This is huge because it pinpoints exactly
how the bacteria interact with a host's immune system.
The idea of beneficial bacteria isn't new, but until
now, the mechanism wasn't clear: "In Europe they sell
probiotics by the gallon, and it's never been shown
scientifically how it's supposed to work," Dr Kasper
says.
Establishing the link between microbe
and mammal may point the way to developing new approaches
to treating IBD. The authors write that "symbiosis factors
such as PSA might potentially provide therapeutics for
human inflammatory disorders on the basis of entirely
novel biological principles." And there may be many
more — as yet unknown — associations between
bacteria and their hosts. For example, imbalances in
the gut microcosmos might also help explain other diseases,
including food allergies and asthma. To date, we know
very little about the microbes that dwell in our intestines:
"There are trillions of bacteria in the human gut, and
we can't even grow most of them," Dr Kasper says.
LOVE
THY MICROBES
While B fragilis is common in the human bowel,
the etiology of colitis in people may differ from that
in mice. For instance, the researchers used the bacterium
Helicobacter hepaticus to induce colitis in the
rodents, but this organism isn't known to have the same
effect in the human gut. Truth is, the causes of IBD
in people aren't well understood at all. The condition
is attributed to an aberrant immune response directed
at normal everyday bacteria in the gut that usual-ly
do no harm. No one's sure why these bacteria are being
targeted.
One popular theory is the 'hygiene
hypothesis,' the idea that a lack of exposure to both
pathogenic and symbiotic microbes in early childhood
adversely affects maturation of the immune system. The
Nature study supports this hypothesis as it shows
that disease — in this case colitis — may
result from the absence of beneficial gut bacteria and
the molecules they produce.
|